East Asian Arch Psychiatry 2012;22:154-9
ORIGINAL ARTICLE
香港叁间药物滥用诊所的咳药水滥用患者其临床特徵:回顾研究
邓嘉林、邓伟光、梁华君、陈虎、麦舜芝、翁礼和
Dr Alan K. Tang, MBBS, FHKAM (Psychiatry), Department of Psychiatry, Prince of Wales Hospital, Hong Kong SAR, China.
Prof. Wai-Kwong Tang, MBChB, MD, FHKAM (Psychiatry), Department of Psychiatry, The Chinese University of Hong Kong, Hong Kong SAR, China.
Dr Huajun Liang, MPhil, Department of Psychiatry, The Chinese University of Hong Kong, Hong Kong SAR, China.
Dr Fu Chan, FHKAM (Psychiatry), Department of Psychiatry, North District Hospital, Hong Kong SAR, China.
Dr Shun-Chi Mak, Department of Psychiatry, Prince of Wales Hospital, Hong Kong SAR, China.
Prof. Gabor Sandor Ungvari, PhD, FRANZCP, FRCPsych, School of Psychiatry & Clinical Neuroscience, University of Western Australia, Perth, Australia.
Address for correspondence: Prof. Wai-Kwong Tang, Department of Psychiatry, 7th Floor, Shatin Hospital, 33 A Kung Kok Street, Ma On Shan, New Territories, Hong Kong SAR, China.
Tel: (852) 2636 7754; Email: tangwk@cuhk.edu.hk
Submitted: 11 June 2012; Accepted: 30 July 2012
Abstract
Objectives: Cough mixture is the third most commonly abused substance in patients attending the Prince of Wales Hospital Substance Abuse Clinic. The content of the local cough mixture is not well researched. Paranoid psychosis manifesting as persecutory delusions and derogatory hallucination, as well as mood symptoms, is common in these patients. The natural history and outcome of such psychoses associated with cough mixture abuse are not well known. This study aimed to address these questions.
Methods: This was a retrospective study of cough mixture abuse in Hong Kong. Case records of cough mixture abusers currently receiving treatment at the 3 substance abuse clinics at the Prince of Wales Hospital, Alice Ho Miu Ling Nethersole Hospital, and the North District Hospital were retrieved for data collection. The patients’ demographic data, duration and intake pattern of cough mixture, and use of any other drugs were documented. The presenting psychopathology, first urine toxicology results, diagnosis, treatment, number of hospitalisations, and course of the illness were also recorded.
Results: A total of 63 patients with the diagnosis of cough mixture abuse were identified in the database; 89% were male. The mean ± SD age of the patients was 34.4 ± 6.2 years; 67% were single and 83% were unemployed. The mean ± SD age of onset of cough mixture abuse was 20 ± 5 years. Psychiatric symptoms developed a mean ± SD of 7.6 ± 6.0 years after onset of abuse. According to the ICD-10 Mental and Behavioural Disorders criteria, the top psychiatric diagnoses were substance-induced psychotic disorder (67%), schizophrenia (19%), depressive disorder (11%), and dysthymia (10%). The most common ingredients in the urine sample at first presentation were promethazine (75%), pseudoephedrine (67%), codeine (60%), ephedrine (57%), zopiclone (17%), and hydrocodone (16%). Additionally, 16% of patients were in the priority follow-up group. The mean ± SD follow-up period was 6.2 ± 7.1 years during which there were 3.2 ± 3.7 episodes of hospitalisations, with a mean ± SD length of stay in each admission of 25.0 ± 40.9 days.
Conclusions: Promethazine, ephedrine, pseudoephedrine, codeine, and hydrocodone are the most common ingredients of cough mixture abused in this locality. Psychotic disorders are the most frequent psychiatric diagnosis associated with cough mixture abuse.
Key words: Psychopathology; Substance-related disorders
摘要
目的:在威尔斯亲王医院药物滥用诊所患者中,咳药水是第叁常见成瘾药物。不过,有关在香港出售的咳药水成份仍未得到透彻研究。这些患者常出现被迫害妄想性或贬抑幻觉性妄想型精神病以及情绪症状,但有关这种精神病其自然史和结果与咳药水滥用的相关性,至今仍缺乏了解。本研究旨在检视这些问题。
方法:回顾香港咳药水滥用情况,并於威尔斯亲王医院、大埔拿打素医院和北区医院这3间药物滥用诊所内,收集正接受咳药水成瘾治疗患者的病例记录,和他们的人口统计学数据、成瘾时间和摄入方式,以及曾否同时滥用其他药物。研究也记录患者的精神病理学、首次尿毒素学测试结果、诊断、治疗、住院次数和病程。
结果:从数据库辨认共63名确诊咳药水滥用患者,当中89%为男性。这患者群组的平均年龄为34.4岁(标準差6.2岁)、67%为单身,待业的则有83%。他们滥用咳药水的始发年龄平均为20岁(标準差5岁),且在滥用咳药水後平均7.6年(标準差7.1年)出现各种精神症状。根据ICD-10精神病学诊断标準,最常见的诊断包括因药物引致的精神异常(67%)、精神分裂症(19%)、抑鬱(11%)和低落性情感病患(10%)。在首次入院进行的尿液测试中,最常见的药物滥用成份包括异丙嗪(75%)、伪麻黄碱(67%)、可待因(60%)、麻黄碱(57%)、佐匹克隆(17%)和氢可酮(16%)。16%患者属优先随访类别。平均随访期为6.2年(标準差 7.1年)、平均住院次数为3.2次(标準差3.7次),平均留院期则为25.0天(标準差40.9天)。
结论:异丙嗪、麻黄碱、伪麻黄碱、可待因和氢可酮为本地滥用咳药水的最常见成份。精神异常是与咳药水滥用相关的最常见精神病学诊断。
关键词:精神病理学、与药物相关的精神异常
Introduction
In the US, up to 4.9% of 12th graders reported lifetime misuse of cough medicine, with 3.7% reporting misuse within the previous 12 months.1 In the 2008/2009 survey of drug use among students conducted by the Narcotics Division in Hong Kong, 2.6% of secondary school students reported any type of illicit drugs misuse within the previous 12 months, of which 26.4% was cough medicine.2 The first reports of cough mixture abuse surfaced in Hong Kong in the 1980s and, by 2011, 4.4% of male substance abusers reported use of cough mixture, as opposed to only 1.8% of female substance abusers.3 Cough mixture is the sixth favourite substance abused after heroin, ketamine, hypnotics, methamphetamine, and cocaine.4
Few studies have focused on the psychopathology associated with cough mixture abuse. Mattoo et al5 conducted a cross-sectional study involving 46 participants who were seeking help from an addiction clinic in North India. In all, 4 were diagnosed with schizophrenia, and 3 each were diagnosed with affective disorder or generalised anxiety disorder. Based on the data from the 2006 National Survey on Drug Use and Health, Ford6 reported elevated risks for major depressive disorder in teenagers misusing cough mixture. Ishigooka et al7 noted a hallucinatory-paranoid state and affective disorders in a series of 44 cough mixture abusers in Japan. In a Hong Kong study of 27 hospitalised cough mixture abusing patients, a significant percentage exhibited severe psychotic and mood disturbances, most commonly persecutory delusions, auditory hallucinations, and depressive symptoms.8
Cough mixture is the third most commonly abused substance in patients attending the substance abuse outpatient clinic at the Prince of Wales Hospital (PWH), Hong Kong.9 Cough mixture misuse frequently presents as mood and psychotic symptoms, but its psychopathology and natural history of the psychosis are not well known. Also, the content in the cough mixture sold in Hong Kong has not been adequately investigated. The objective of the present study was therefore to examine these factors.
Methods
Study Population
The medical records of patients, with a diagnosis of cough mixture dependence according to the ICD-10 Mental and Behavioural Disorders10 criteria who attended the substance abuse clinics of the PWH, Alice Ho Miu Ling Nethersole Hospital, and North District Hospital from October 2009 to December 2011, were reviewed. These 3 substance abuse clinics serve the entire Northeastern area of Hong Kong with a population of approximately 1.2 million, constituting about one-sixth of the total population.11
The study was conducted in compliance with the Declaration of Helsinki. The study protocol was approved by the Joint Chinese University of Hong Kong–New Territories East Cluster Clinical Research Ethics Committee. Written informed consent is not required for this type of retrospective study as the collection of information is part of routine clinical care.
Data Collection
Standard clinical case records of patients attending for cough mixture misuse at the 3 clinics were retrieved for data collection. Demographic data including sex, age, education, marital status, employment, and forensic record were extracted. The history of cough mixture use, age of onset, maximum and recent amount of cough mixture abused, and history of detoxification were documented, together with the use of any other substances. The following clinical characteristics were recorded: age of onset of psychiatric symptoms, psychopathology, psychiatric diagnosis, duration between cough mixture consumption and appearance of first psychiatric symptoms, total number of hospitalisations, current treatment, and the latest Christo Inventory of Substance-misuse Services (CISS)12 score. The CISS was developed as a single-page outcome evaluation tool completed by drug / alcohol service workers. The CISS consists of 10 items reflecting clients’ problems with social functioning, general health, sexual / substance risk- taking behaviour, psychological functioning, occupation, criminal involvement, drug / alcohol use, ongoing support, compliance, and working relationships. The ingredients of the cough mixture were determined at the first urine toxicology test.
Statistical Analysis
The data were analysed using the Statistical Package for the Social Sciences, Windows version 15.0 (SPSS Inc, Chicago [IL], US). Socio-demographic and clinical characteristics of the participants were presented as descriptive statistics. Regression analysis was employed to evaluate the clinical characteristics against CISS scores. The results are presented as mean ± standard deviation (SD).
Results
A total of 63 patients were identified as being cough mixture misusers at the 3 clinics during the study period of October 2009 to December 2011. Their case notes were retrieved and reviewed. The mean ± SD age of the group was 34.4 ± 6.2 years; 56 (89%) subjects were male; 67% were single; the mean ± SD duration of education was 8.7 ± 1.4 years; 83% were unemployed for a mean ± SD of 4.4 ± 5.7 years; and 67% used to work in the service sector. Approximately 75% had a forensic record; among these, 32% had drug- related offences, 13% had non–drug-related offences, 24% had both, and data of the remainder (6%) were missing (Table 1).
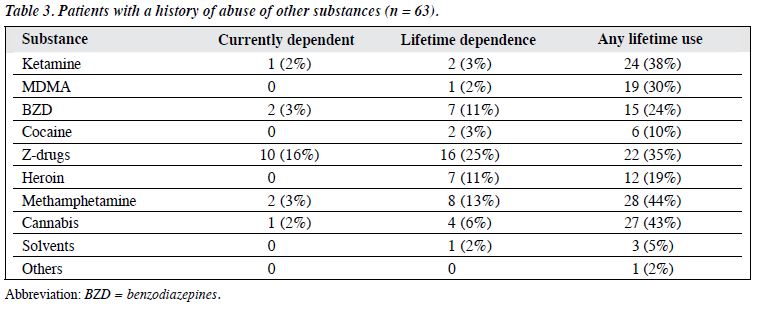
The history of cough mixture abuse of participants is shown in Table 2. They first experimented with illicit substances at a mean ± SD age of 18 ± 5 years and started cough mixture abuse at a mean ± SD age of 20 ± 5 years, reaching a mean ± SD maximum consumption of 2.3 ± 1.6 bottles/day by a mean ± SD age of 24 ± 6 years. When the participants attended the clinic, the mean ± SD amount consumed decreased to 0.6 ± 0.8 bottle/day. The favourite venue for consumption was video game centres (25%) followed by their home (21%) and the pharmacy where the drug was purchased (11%). Multiple substance abuse was also common (Table 3). Close to 16% of the participants were actively co-dependent on the so-called ‘Z-drugs’ (including zopiclone or zolpidem), and about one-quarter reported a history of dependence on Z-drugs as well as sedative hypnotics (11%), heroin (11%), or methamphetamine (13%).
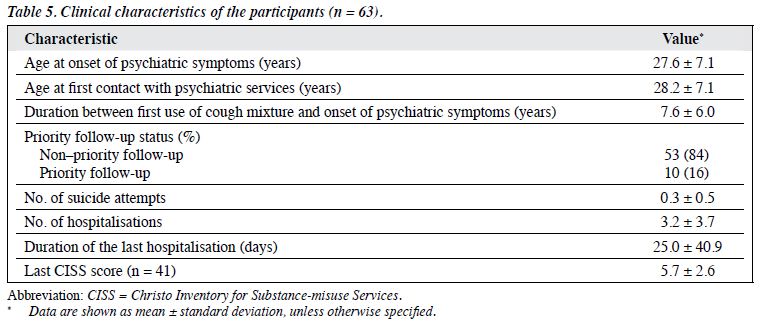
The clinical characteristics of participants are shown in Tables 4 and 5. The most common psychiatric diagnoses were substance-induced psychotic disorder (67%), schizophrenia (19%), depressive disorders (11%), and dysthymia (10%). The respective mean ± SD age of onset of psychiatric symptoms and first contact with the psychiatric services was 27.6 ± 7.1 and 28.2 ± 7.1 years, and there was a mean ± SD of 3.2 ± 3.7 episodes of psychiatric hospitalisations. The mean ± SD CISS score of the 41 participants who were rated on this scale (i.e. new cases at their first visit to the clinic) was 5.7 ± 2.6. Among them, 26 (63%) participants scored ≤ 6 and 15 (37%) scored ≥ 7. Additionally, 16% of patients were in the priority follow-up group. The mean ± SD follow-up period was 6.2 ± 7.1 years.
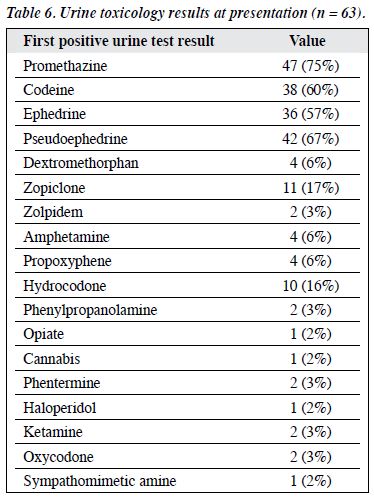
Concerning the ingredients of the local cough mixture, dextromethorphan was only detected in 6% of the urine samples. The most frequently detected substances were promethazine (75%), pseudoephedrine (67%), codeine (60%), ephedrine (57%), zopiclone (17%), and hydrocodone (16%) [Table 6].
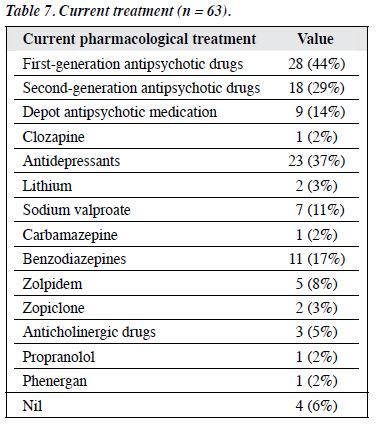
The current treatment regimens are shown in Table 7. Most participants (73%) were taking antipsychotic medication. Besides, 14% of the subjects were on depot medication. Additionally, 37% of participants received antidepressants, 17% were taking benzodiazepines, and 11% took Z-drugs.
Discussion
Compared with other over-the-counter cough medicines available elsewhere,13-16 dextromethorphan was not a common ingredient in the cough medicine sold in Hong Kong. In Hong Kong, ephedrine and pseudoephedrine are frequent ingredients in commercially available cough medicines, similar to other Asian countries including India,5Thailand,17 Taiwan,18 Japan,7,19 and Singapore.20
Cough mixture is usually bought from pharmacies and consumed immediately. Similar to the findings of another Hong Kong study,21 many users reported consumption in video game centres before enjoying a round of video games. They felt cough mixture gave them superior concentration and improved their focus and confidence.
Similar to other Asian locations, in Hong Kong most cough mixture abusers are unemployed men who started taking the substance in their teenage years. In an Indian study,5 all 46 participants were male, with a mean age of starting cough mixture abuse of 22.7 years. In another Indian report from the area of Assam and Nagaland,22 the respective mean age of onset of abuse for the 97 patients was 17.4 and 15.8 years; all were male, over 90% were single, and 62.5% in Assam and 97.9% in Nagaland were unemployed.
It would appear that female cough mixture abusers are uncommon across Asia. In this study, 11% of the participants were women and the figure was 22.2% in a previous Hong Kong study,8 while none of the other mentioned Asian studies reported any female cough mixture abusers. In most countries of the world, particularly in developing countries, women’s lives are very different from those of men. Substance misuse in women is often more stigmatised and carries extreme condemnation from society. Women’s access to treatment is hindered by cultural taboos and clashes with childcare responsibilities.23 It is likely that substance abuse among women is grossly under-reported and under-treated. A study conducted by the United Nations on substance misuse in Asian women described a series of 75 women recruited through snowball sampling in India.24 The authors concluded that barriers to treatment included concerns for children unattended at home, fear of exploitation, fear of withdrawal, and lack of support systems. Heroin was the most commonly abused substance in that series, but several female cough mixture abusers were also found; however, it was not known if they received any treatment.
Similar to the results of this study, psychotic syndromes were the most frequent psychiatric co-morbidities in the Indian5 and Japanese studies.7 The frequency of psychiatric diagnoses was almost identical with that of the other local study,8 where diagnoses included substance- related psychotic disorders (60%), schizophrenia (15%), major depressive episode (4%), and personality disorder (4%). As expected, psychotic disorders were the most common conditions seen at the substance abuse clinics.
Ephedrine and pseudoephedrine use has been known to be related to psychoses. Since a significant proportion of the patients in this study misused multiple substances, which may have included other, more potent, stimulants such as methamphetamine, the contribution of the cough mixture ingredients to the development of psychoses remains unclear. Most participants developed a psychiatric disorder after some years of abuse. In this study, a gap of 7 years lapsed between the first use of cough mixture and the development of psychiatric symptoms. Based on the findings of this study, it is conceivable that the risk of cough mixture abusers developing a psychosis may be elevated with increased total lifetime abuse.
In the Hong Kong study,8 the participants admitted concomitant use of benzodiazepines (56%), cannabis (33%), cocaine (15%), heroin (15%), hallucinogens (11%), and solvents (7%). In the study by Mattoo et al,5 concurrent use of other substances was reported in 72% of participants, and were most commonly benzodiazepines (42%), opioids (12%), alcohol (10%), or combinations of these and / or carisoprodol (36%), a muscle relaxant with sedative properties. These figures are quite different from the findings on co-dependence of this study: 16% were concurrently dependent on Z-drugs, 3% each for methamphetamine and benzodiazepines, and 2% each for ketamine and cannabis. Zopiclone was the co-dependent substance with cough mixture most frequently detected in 17% of the participants. Zopiclone’s popularity may be explained by the fact that it is often purchased together with cough mixture in the pharmacy, often at a discount. Reflecting the change of times, the use of ketamine in this study was more prevalent than in the mid-1990s, with 38% of the participants reporting any lifetime use, although only 3% were apparently dependent on ketamine. With a lifetime dependence of 25%, Z-drugs remained the most commonly abused substances to be co-dependent with cough mixture in Hong Kong.
There are several limitations of the study. First, the participants were receiving tertiary care, thus the findings may not be generalisable to the entire substance abuse population, a significant proportion of whom might not be in treatment. Second, although the data were collected by the principal investigator, the diagnoses were established through clinical interviews and not with the aid of structured clinical interviews. Third, co-morbid multiple substance misuse is common in cough mixture abusers, it is therefore difficult to know whether a particular psychiatric condition is related to cough mixture per se, or related to other substances, or a combination of both. In fact, the composition of the cough mixture was not uniform; whether ephedrine or pseudoephedrine was the offending agent responsible for inducing psychiatric disorders remains uncertain.
Conclusions
Psychotic disorders were the most common psychiatric diagnosis in cough mixture–dependent patients attending 3 substance abuse clinics in Hong Kong. Common ingredients in local cough mixture were promethazine, ephedrine, pseudoephedrine, codeine, and hydrocodone, while dextromethorphan was infrequently detected. Co- dependence of cough mixture with zopiclone or zolpidem was often found.
References
- Falck R, Li L, Carlson R, Wang J. The prevalence of dextromethorphan abuse among high school students. Pediatrics 2006;118:2267-9.
- The 2008/09 Survey of Drug Use among Students. Hong Kong SAR Government Narcotics Division, Security Bureau Website: http://www.nd.gov.hk/en/survey_of_drug_use.htm. Accessed 11 Sep 2011.
- Table 16. Reported drug abusers by age group by sex by common type of drugs abused. Central Registry of Drug Abuse website: http://www.nd.gov.hk/statistics_list/doc/en/t16.pdf. Accessed 9 Sep 2011.
- Table 3. Newly/previously reported drug abusers by age group by common type of drugs abused. Central Registry of Drug Abuse website: http://www.nd.gov.hk/statistics_list/doc/en/t3.pdf. Accessed 11 May 2012.
- Mattoo SK, Basu D, Sharma A, Balaji M, Malhotra A. Abuse of codeine-containing cough syrups: a report from India. Addiction 1997;92:1783-7.
- Ford JA. Misuse of over-the-counter cough or cold medications among adolescents: prevalence and correlates in a national sample. J Adolesc Health 2009;44:505-7.
- Ishigooka J, Yoshida Y, Murasaki M. Abuse of “BRON”: a Japanese OTC cough suppressant solution containing methylephedrine, codeine, caffeine and chlorpheniramine. Prog Neuropsychopharmacol Biol Psychiatry 1991;15:513-21.
- Lam LC, Lee DT, Shum PP, Chen CN. Cough mixture misuse in Hong Kong — an emerging psychiatric problem? Addiction 1996;91:1375-8.
- Tang A, Liang HJ, Ungvari GS, Tang WK. Referral patterns and clinical characteristics of subjects referred to substance abuse clinic of a regional hospital in Hong Kong. East Asian Arch Psychiatry 2011;21:22-7.
- World Health Organization. The ICD 10 Classification of Mental and Behavioral Disorders. Geneva: WHO; 1992.
- 2011 Population Census Results. Website: http://www.census2011. gov.hk/en/district-profiles.html. Accessed 9 May 2012.
- Christo G, Spurrell S, Alcorn R. Validation of the Christo Inventory for Substance-misuse Services (CISS): a simple outcome evaluation tool. Drug Alcohol Depend 2000;59:189-97.
- Darboe MN. Abuse of dextromethorphan-based cough syrup as a substitute for licit and illicit drugs: a theoretical framework. Adolescence 1996;31:239-45.
- Elwood WN. Sticky business: patterns of procurement and misuse of prescription cough syrup in Houston. J Psychoactive Drugs 2001;33:121-33.
- Manaboriboon B, Chomchai C. Dextromethorphan abuse in Thai adolescents: a report of two cases and review of literature. J Med Assoc Thai 2005;88 Suppl 8:S242-5.
- Miller SC. Dextromethorphan psychosis, dependence and physical withdrawal. Addict Biol 2005;10:325-7.
- Chomchai C. Stimulant methamphetamine and dextromethorphan use by the Thai youth [abstract]. Proceedings of the 10th Scientific Congress of the Asia Pacific Association of Medical Toxicology; 2011 Nov 12-14. Website: http://www.asiatox.org/10thAPAMT/Stimulant%20methamphetamine%20and%20dextromethorphan%20use%20by%20the%20Thai%20youth.pdf. Accessed Jun 2012.
- Liu C, Li JH, Tsay WI, Hsu J. Drug use and profile of individuals arrested on drug-related charges in Taiwan. J Food Drug Anal 2005;13:101-6.
- Suzuki T, Masukawa Y, Misawa M. Drug interactions in the reinforcing effects of over-the-counter cough syrups. Psychopharmacology (Berl) 1990;102:438-42.
- Ong B, Cheah JS. Codeine cough mixture addiction mimicking thyrotoxicosis. Singapore Med J 1985;26:494-5.
- Shek DT. Cough medicine abuse among young people in Hong Kong. International Conference on Tackling Drug Abuse — Conference Proceedings. Website: http://www.nd.gov.hk/en/conference_proceedings/ Drugs_proBK_Part2/Drugs_proBK_Daniel.pdf. Accessed Jun 2012.
- Wairagkar NS, Das J, Kumar S, Mahanta J, Satyanarayana K, Phukan RK, et al. Codeine containing cough syrup addiction in Assam and Nagaland. Indian J Psychiatry 1994;36:129-32.
- Reid G, Costigan G. Revisiting ‘The Hidden Epidemic’. A situation assessment of drug use in Asia in the context of HIV/AIDS. Fairfield, Australia: Centre for Harm Reduction/Burnet Institute; 2002.
- Murthy P. Women and drug abuse: the problem in India. India, Ministry of Social Justice and Empowerment/United Nations International Drug Control Programme, Regional Office for South Asia; 2002.